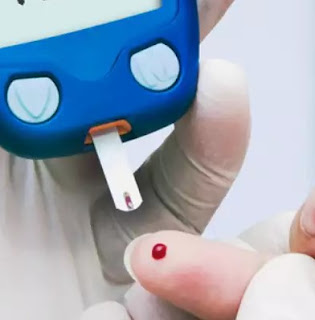
Diabetes mellitus is a chronic condition where the body either does not produce enough insulin or fails to use insulin effectively, leading to elevated blood glucose levels. Insulin, a hormone produced by the pancreas, is essential for regulating blood sugar by allowing cells to absorb glucose for energy. In type 2 diabetes, the body’s cells become resistant to insulin, causing sugar to accumulate in the bloodstream because cells cannot utilize it efficiently. This condition is exacerbated by factors such as obesity, sedentary lifestyle, and genetic predisposition.
Conversely, excessive insulin can result in hypoglycemia, where too much glucose enters the cells, leaving insufficient glucose in the bloodstream. This can occur due to an overdose of insulin or other medications that increase insulin levels, excessive alcohol consumption, or missed meals. When blood glucose levels drop too low, it triggers symptoms like nervousness, irritability, hunger, headache, shakiness, rapid heartbeat, and weakness. These symptoms reflect the brain's urgent need for glucose, as it relies on it as a primary energy source.
Effective management of diabetes involves maintaining blood glucose levels within a target range through a balanced diet, regular physical activity, medication, and regular monitoring. Advances in continuous glucose monitoring (CGM) and insulin pump technologies have significantly improved diabetes management, allowing for better control and reducing the risk of complications such as cardiovascular diseases, neuropathy, and retinopathy. Regular consultations with healthcare providers are crucial to tailor treatment plans and ensure optimal health outcomes for individuals with diabetes.
Balancing Blood Sugar: Understanding and Managing Diabetes Mellitus
The Evolution of Modern Food Flavor
-
The evolution of modern food flavor is a story shaped by scientific
curiosity, technological progress, and the growing demands of an
industrialized world. ...